Get the full story of the microbiome
- Importance of Microbial Diversity
- Dysbiosis and Recurrent C. difficile Infection
- Historic Microbiome Restoration Approaches
- Patient and Healthcare Burdens
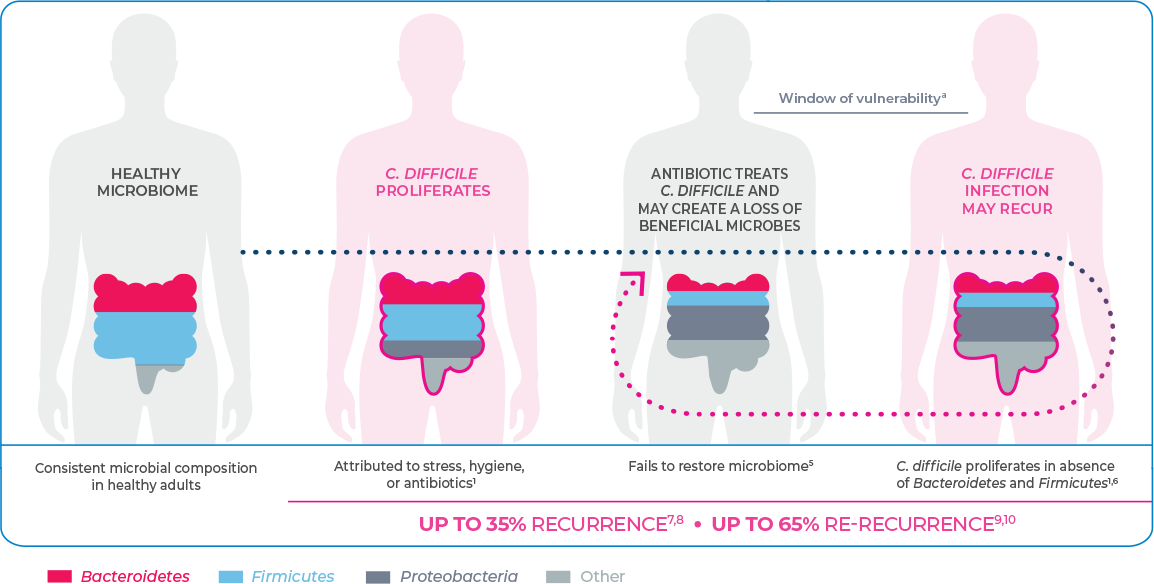
C. difficile may proliferate as a result of dysbiosis
Dysbiosis creates an insufficiency of Bacteroidetes and Firmicutes, which may lead to an environment suited for the growth of C. difficile infection (CDI).1,2
Dysbiosis is the disruption of the volume and diversity of the gut microbiome. This may be attributed to factors including stress, diet, hygiene, and antibiotic use. Dysbiosis is associated with a range of gastrointestinal (GI) and non-GI diseases including neurologic, metabolic, liver, inflammatory, and infectious diseases.1,3,4
The gut microbiota generally play a role in colonization resistance by which the native organisms prevent pathogenic microbes from flourishing. Disruption of the gut microbiome leads to an environment suited for the proliferation of C. difficile.1,2